- Deep Brain Stimulation Surgery Pictures
- What is Deep Brain Stimulation Surgery?
- DBS System Diagrams: What Do They Look Like?
- Deep Brain Stimulation Surgery Pictures
- Before and After Deep Brain Stimulation Surgery
- Clinical Indications of DBS Surgery
- Best Candidates for DBS Surgery (Age, Severity and Health)
- How Successful is DBS Surgery?
- Why Choose Turkey for Deep Brain Stimulation in 2026?
- Trust Turkey Luxury Clinics for Precise DBS Surgery and Close Monitoring
- FAQs About DBS Pictures
Viewing images that showcase the entire Deep Brain Stimulation (DBS) surgery, from electrode placement to pulse generator implantation and final programming, offers a clear visual understanding of how this advanced system works and its role in managing neurological symptoms.
At Turkey Luxury Clinics, we use detailed pictures to explain the DBS device, its effects, the surgical steps, and what patients can expect, helping answer key questions and make the process easier to understand.
Deep Brain Stimulation Surgery Pictures
Deep Brain Stimulation (DBS) surgery involves the precise placement of electrodes in targeted brain regions and connection to a small pulse generator implanted under the chest skin. Viewing images of DBS surgery, from stereotactic frame setup, lead implantation, to pulse generator insertion, provides a clear visual understanding of the procedure. These pictures illustrate how each component works together to deliver controlled electrical stimulation, helping manage movement and neurological disorders effectively.
What is Deep Brain Stimulation Surgery?
Deep Brain Stimulation (DBS) is a neurosurgical procedure used to treat movement and neurological disorders by implanting electrodes into targeted brain regions and connecting them to a small pulse generator under the skin.
DBS System Diagrams: What Do They Look Like?
A Deep Brain Stimulation (DBS) system diagram shows a device made up of multiple components, some implanted inside the body and others used for external control.
Working as a brain pacemaker, the DBS system consists of three main components: electrodes placed in the brain, extension wires running under the skin, and an Implantable Pulse Generator (IPG) placed in the chest. It treats movement disorders by sending electrical pulses to specific brain regions to regulate abnormal neural signals.
Pictures Illustrate the Components of the DBS System
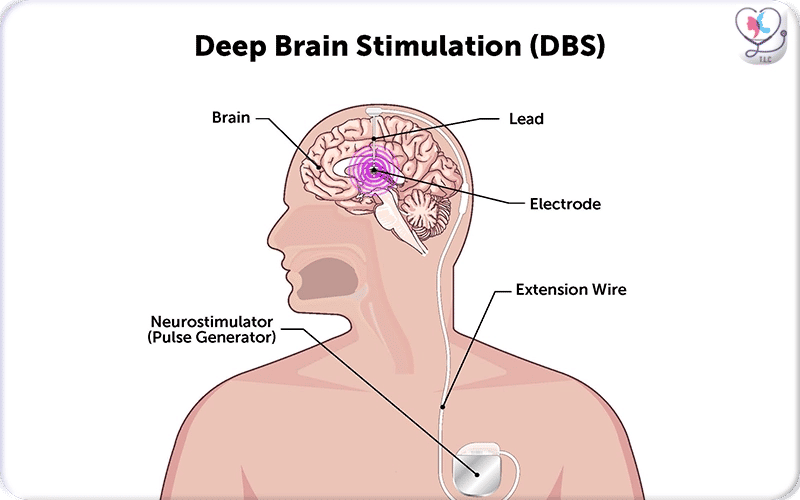
Illustration of Deep Brain Stimulation (DBS): electrodes implanted deep in the brain are connected via insulated leads to a neurostimulator (pulse generator) placed under the skin — allowing targeted electrical stimulation to regulate abnormal neural activity.
Components of a DBS System Diagram
1. Electrodes (Leads): Thin, insulated wires with four small contacts at the tip, inserted into specific target areas deep within the brain. DBS electrodes come in different sized and length for diverse effects and cases control:
- Electrode size: determines stimulation spread; larger electrodes cover wider areas but with less precision, while smaller ones are more precise but more limited in range.
- Length: affects access to deeper brain regions and the ability to target multiple neural levels.
- Contact spacing: controls how precisely the stimulation target can be selected within the brain.
- Metal presence in the brain: causes only minor electrical distortion but does not significantly affect recording accuracy or stimulation effectiveness.
2. Extension Wire: A wire that runs under the skin from the scalp, down the neck, connecting the electrode to the IPG in the chest.
3. Implantable Pulse Generator (IPG): A battery-powered, pacemaker-like device placed under the skin, usually below the collarbone. It sends continuous electrical pulses to the brain.
4. Programmer (External): A device used by clinicians to adjust the stimulation parameters (voltage, frequency, pulse width) to optimize symptom control.
DBS Electrical Pulses Pathway Diagram
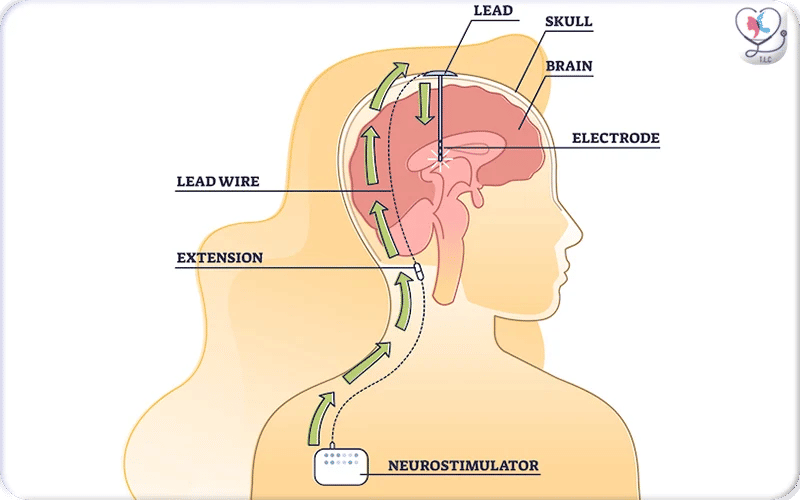
This illustration highlights how electrical pulses travel through the DBS system: the neurostimulator in the chest generates signals that pass through the extension wires and reach the implanted brain electrodes. These signals help stabilize abnormal activity responsible for symptoms such as tremors, rigidity, and slowness, allowing patients to regain smoother and more predictable movement without destroying any brain tissue.
Detailed Deep Brain Stimulation Electrode Brain Diagrams
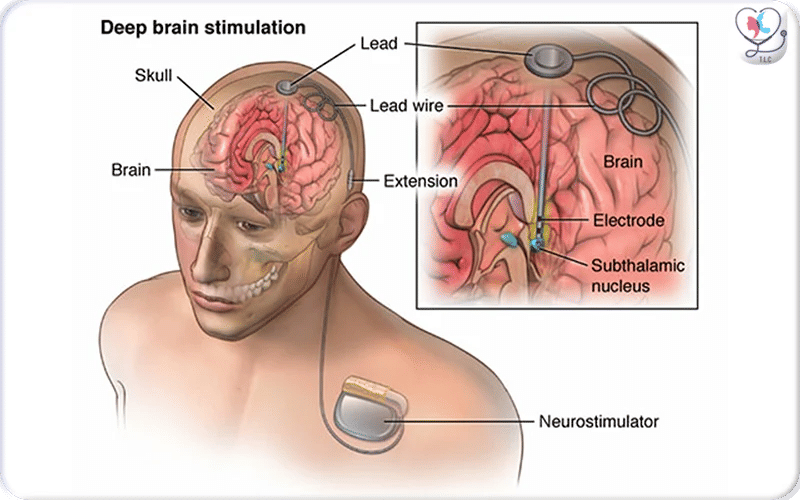
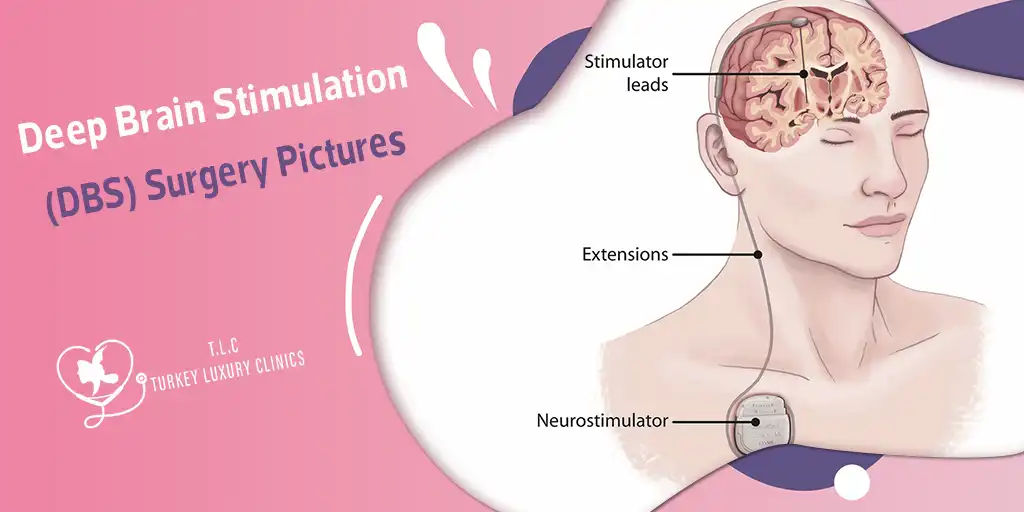
Medical illustration showing the internal components of a Deep Brain Stimulation (DBS) system. A thin electrode is implanted in a specific target area of the brain, connected through extension wires to a neurostimulator placed under the skin in the chest. The device delivers continuous, programmable electrical stimulation, and can be externally adjusted by clinicians to match the patient’s changing needs and optimize symptom control.
Schematic diagram of DBS surgery showing electrode placement, connection through extension wires, and implantation of the pulse generator in the chest for controlled stimulation.
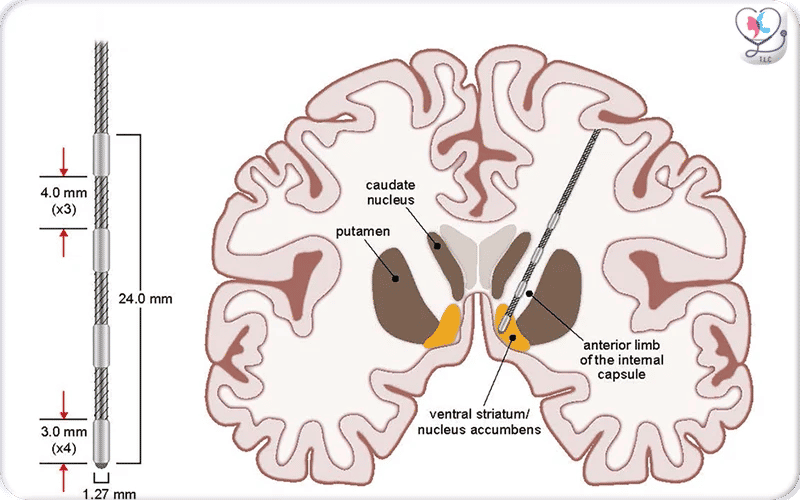
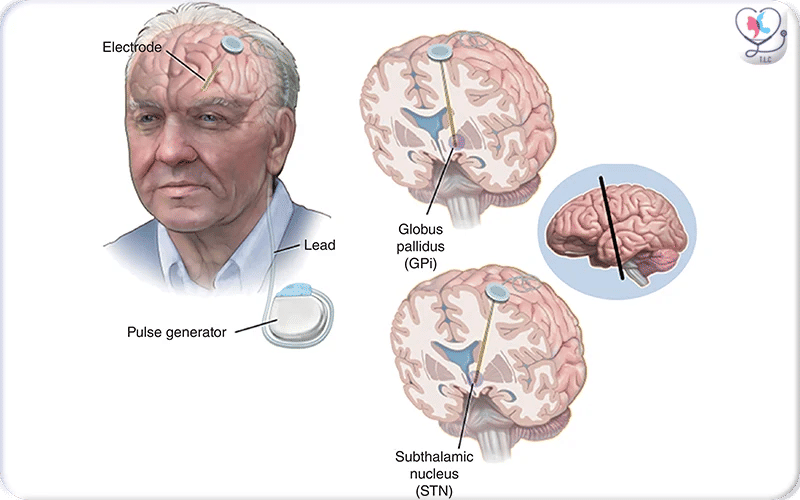
Coronal schematic of the brain showing the implanted stimulating electrode targeting the ventral capsule/ventral striatum (VC/VS), highlighting the deep-brain placement of the lead used in DBS therapy
Deep Brain Stimulation Electrode Positioning Illustration for Different Cases
Subthalamic Nucleus (STN): A common target for Parkinson’s disease, especially effective in improving tremor, rigidity, and bradykinesia.
Globus Pallidus Internus (GPi): Used in Parkinson’s disease and dystonia. GPi is often selected as an alternative to STN, depending on the symptom profile.
Ventral Intermediate Nucleus (VIM) of the Thalamus: Primarily targeted for essential tremor, with strong effectiveness in reducing action and postural tremors.
How Does the DBS System Work for Neurological Disease? Expert Explanation
Dr. Okish, a Board-Certified Neurosurgeon specializing in functional neurosurgery, explains how the Deep Brain Stimulation (DBS) system, used for neurological disorders such as Parkinson’s disease and other movement disorders, the electrodes in specific targeted areas of the brain, while the Implantable Pulse Generator (IPG) is implanted in the chest and controlled through programmed settings.
The electrical impulses are generated by the IPG, then travel through extension wires placed under the skin. These signals reach the electrodes in the brain, which deliver stimulation to specific regions. This stimulation helps regulate abnormal brain activity and reduces movement-related symptoms.
Deep Brain Stimulation Surgery Pictures
DBS surgery is usually performed in two major steps. First, the electrodes are implanted in the targeted brain region and connected to an extension wire beneath the scalp. In the second stage, a pulse generator similar to a pacemaker is placed in the chest and attached to the extension wire. After surgery, the doctor programs the pulse generator to deliver customized electrical stimulation that best controls the patient’s symptoms.
1. Determination of the Site of Lead Placement
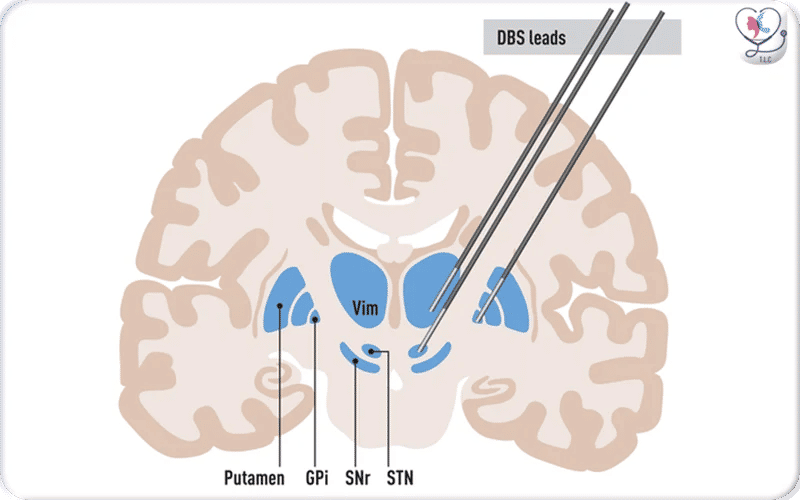
The image shows an anatomical diagram of the basal ganglia and thalamus with three deep brain stimulation (DBS) leads placed in their typical treatment targets. One lead is positioned in the VIM, which is commonly used for tremor control, another in the STN, and a third in the GPi — both of which are key targets for treating Parkinson’s disease and other movement disorders.
Before your DBS surgery, the neurosurgeon needs to determine where the electrodes will be placed depending on the treated condition and affected brain area. usually by using pre surgical MRI. Electrode locations and numbers vary by type of disease and symptoms. This step is crucial for optimal results.
2. DBS Frame, Drill, and Incision Making
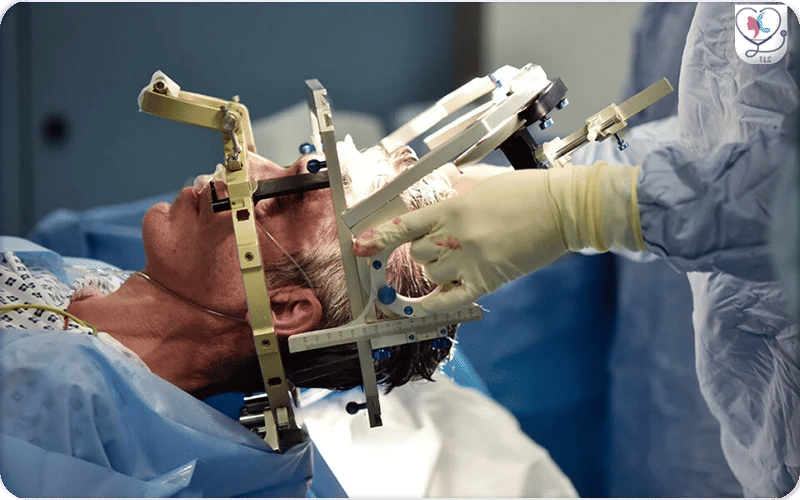
The image shows the patient’s head secured in a DBS stereotactic frame. Surgical instruments are positioned for a precise skull opening (small craniotomy), enabling careful electrode insertion while minimizing risk and ensuring accuracy.
To ensure precise electrode placement, your head is fixed using a stereotactic frame. The surgeon then makes a very thin opening using a drill, allowing safe insertion of electrodes into the targeted brain areas.
3. Lead Implantation (Awake vs Asleep)
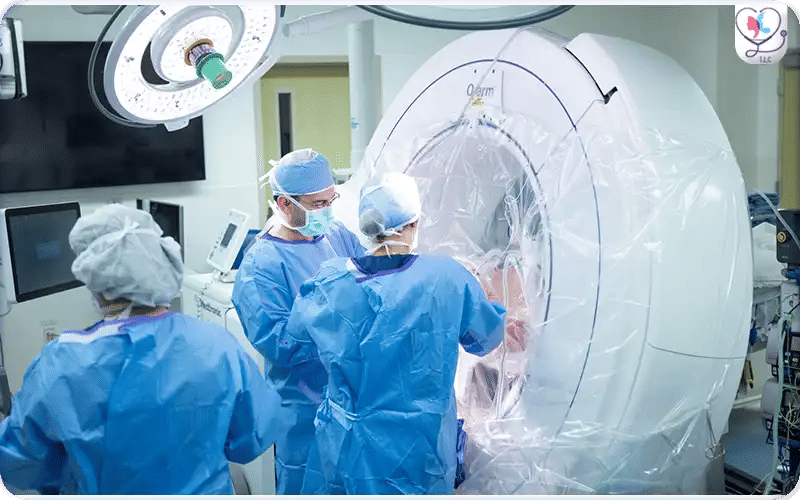
Intraoperative view of a patient undergoing DBS surgery — showing surgical positioning and equipment during lead implantation.
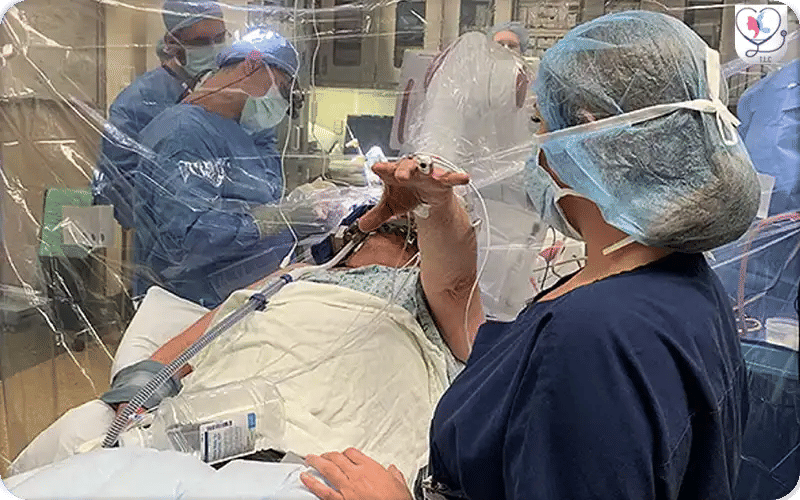
This intraoperative photo shows a patient awake during DBS surgery, raising their hand while the neurosurgeon touches a finger to test responsiveness. This step allows the surgical team to confirm accurate electrode placement in the brain, ensuring optimal stimulation and symptom relief. Awake testing is a crucial part of the procedure for safety and effectiveness.
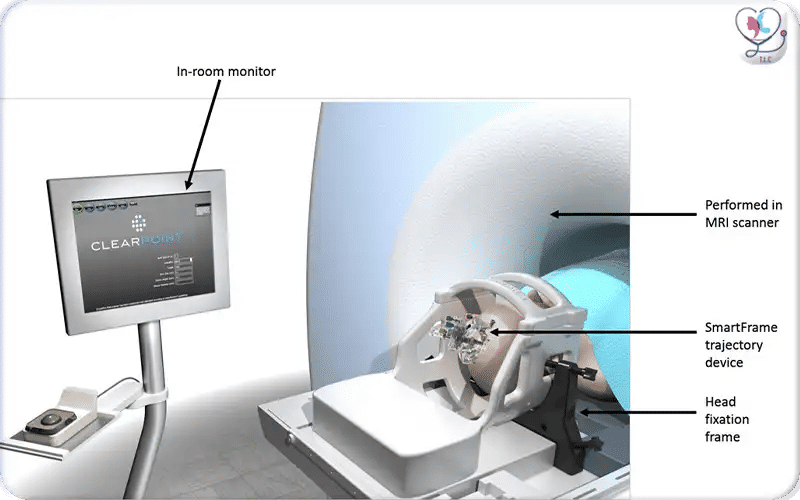
Illustration of ClearPoint MRI-guided DBS with skull-mounted stereotactic frame and trajectory device for precise electrode placement under real-time imaging.
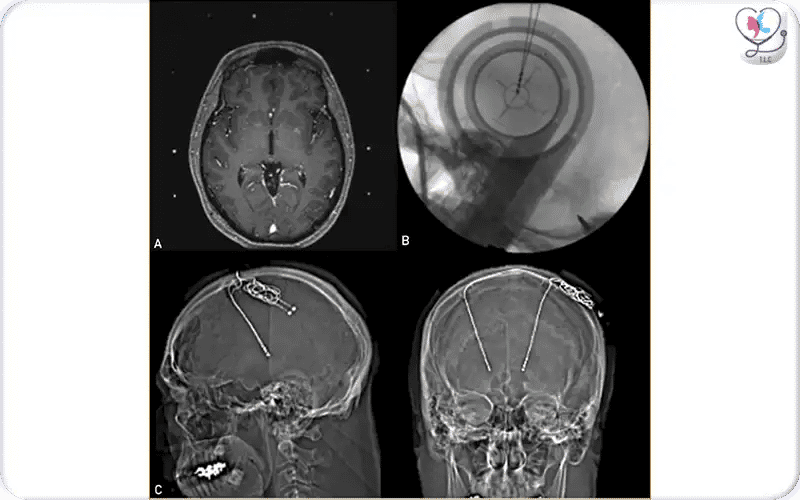
This image shows the use of imaging during DBS surgery. Intraoperative MRI (A) helps the surgeon plan the exact placement of electrodes in the thalamus to treat essential tremor. Fluoroscopy (B) confirms accurate positioning of the electrodes during surgery, and postoperative CT scans (C) verify their final placement, ensuring safe and effective stimulation.
Recent studies show that asleep-DBS can provide similar or better outcomes than awake-DBS for speech, cognitive function, and patient comfort. Modern MRI/iMRI/CT guidance allows precise electrode placement without relying on patient feedback. Awake-DBS is still performed in specialized centers for real-time testing of neurological function.
4. Pulse‑Generator Implantation
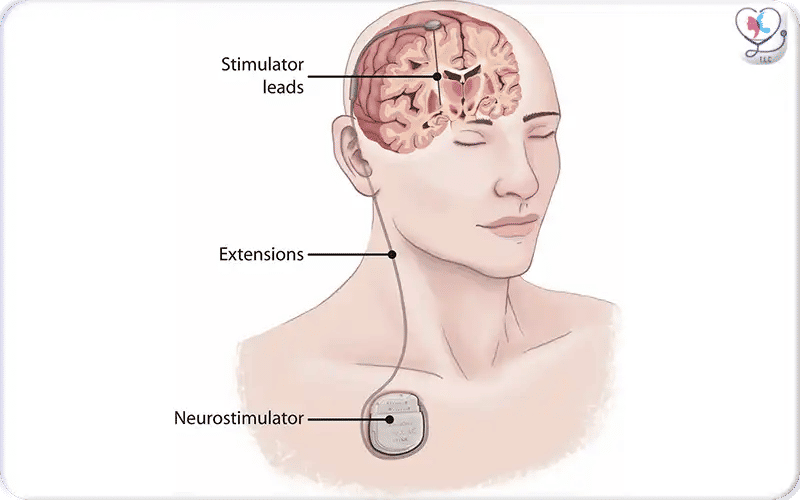
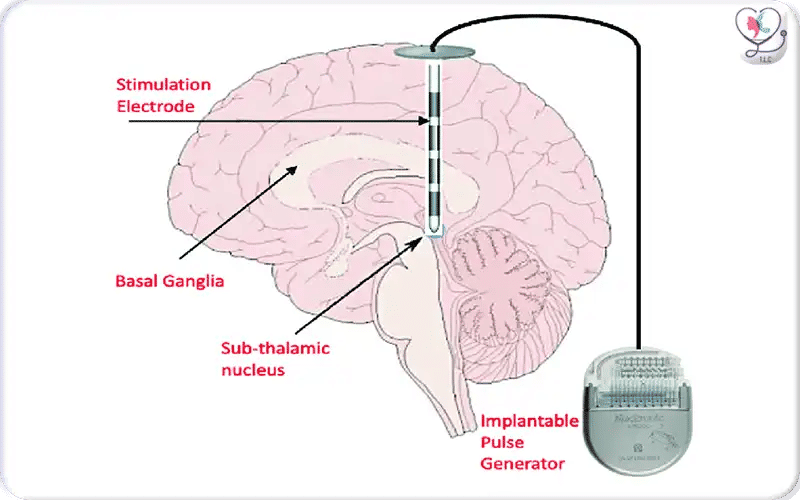
DBS pulse generator implanted under the chest skin, connected via extension wires to brain electrodes, delivering controlled electrical stimulation.
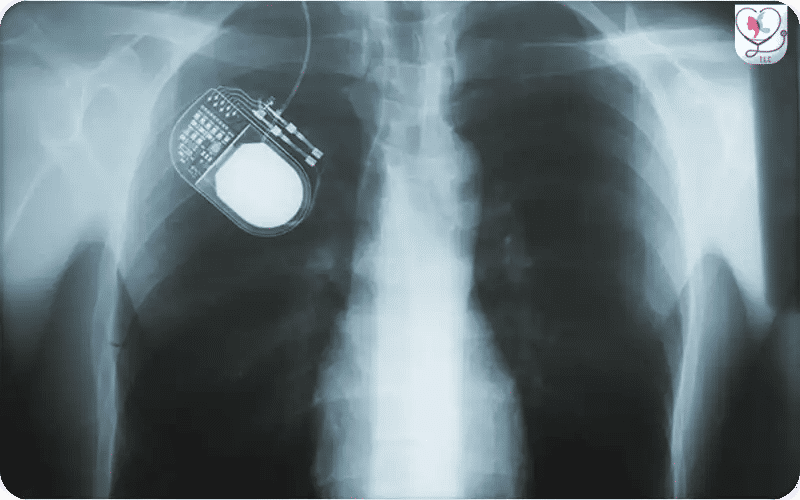
X-ray view of a Deep Brain Stimulation (DBS) system showing the pulse generator implanted in the chest. The extension wire travels up the neck and connects to the intracranial electrodes, providing a detailed technical perspective of the full hardware configuration within the patient.
During the Deep Brain Stimulation (DBS) procedure, the pulse generator—a small, battery-powered device—is implanted under the skin, usually in the upper chest area. This device connects to the electrodes placed in the brain via a thin extension wire, enabling controlled electrical stimulation to manage neurological symptoms.
5. Programming and Activation
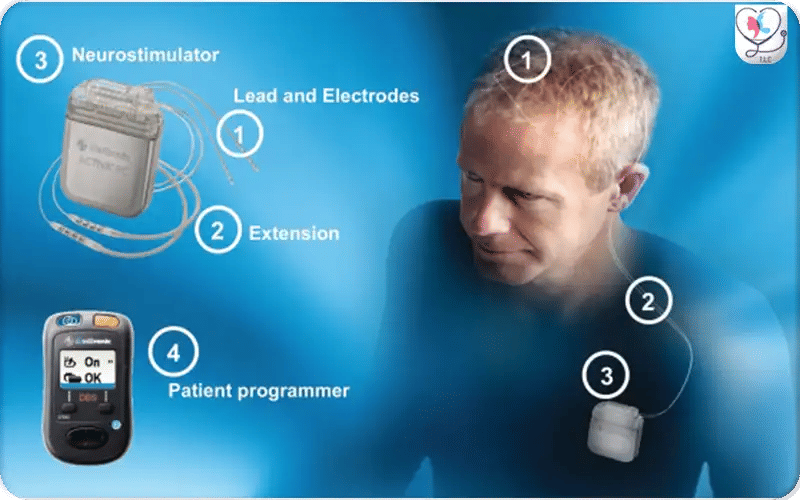
This image shows the programming setup for a DBS system. Clinicians use the patient programmer to adjust stimulation parameters, fine-tuning the device for symptom relief and patient comfort.
After the pulse generator is implanted, the DBS system is programmed and activated. A neurologist or trained clinician uses a patient programmer or specialized device to adjust the stimulation settings. This process ensures the electrical impulses are tailored to the patient’s symptoms, optimizing symptom control while minimizing side effects.
Before and After Deep Brain Stimulation Surgery

The image highlights how targeted electrical stimulation helps reduce tremors and improve motor control, demonstrating the therapeutic impact of the implanted DBS system.
DBS can significantly improve symptoms such as tremors, rigidity, and slow movements. Before surgery, patients may experience noticeable hand tremors, stiffness, and difficulty with everyday tasks. After DBS activation, images often show smoother, more controlled movements, with a marked reduction in tremors and improved motor coordination. Patients frequently report easier hand control and a reduction in involuntary movements, which can greatly enhance daily functioning and quality of life.
Clinical Indications of DBS Surgery
- Parkinson’s Disease (PD):
- Patients experiencing motor fluctuations, dyskinesia (involuntary movements), or tremors that persist despite optimized medication therapy.
- Essential Tremor (ET):
- Individuals with severe, disabling tremor affecting the hands, head, or voice that does not respond adequately to medication.
- Dystonia:
- Patients with generalized dystonia (abnormal muscle contractions and postures) who have not responded well to medical treatment.
- Other Potential Conditions:
- In selected cases, DBS may also be considered for Tourette syndrome, chronic pain, and treatment-resistant obsessive-compulsive disorder (OCD).
- Sources include clinical guidance from organizations such as the National Institute of Neurological Disorders and Stroke (NINDS).
Best Candidates for DBS Surgery (Age, Severity and Health)
- Diagnosed with Parkinson’s disease for 5 years or more
- In mid-stage disease with medication fluctuations or side effects
- Symptoms improve with levodopa is powerful indicator for better DBS results)
- Severe tremor not controlled by medication including Essential tremor
- Experience “off” periods or dyskinesia
- Good memory and stable mental health
- Generally under 75 or in good overall health
- Fit for surgery (no major heart, lung, or bleeding issues)
Who should avoid DBS Surgery?
- Atypical Parkinsonism: Conditions like MSA or PSP.
- Advanced Dementia: High risk of post-operative confusion.
- Severe Brain Atrophy: Visible on MRI, making lead placement risky.
- Active Suicide Ideation: Or unstable psychiatric conditions.
How Successful is DBS Surgery?
Deep Brain Stimulation (DBS) is a highly effective treatment for movement disorders in carefully selected patients. It is not a cure, but it can significantly reduce symptoms and improve daily function and quality of life. Overall success rates are commonly reported around 70–80% improvement in motor symptoms, depending on the condition and patient selection.
DBS Surgery Success Rates by Condition
Condition | Main Improvement | Results Range |
Parkinson’s disease | Tremor reduction | 60–90% |
Parkinson’s disease | Dyskinesia reduction | 70–80% |
Parkinson’s disease | Motor function (UPDRS improvement) | 30–60% |
Essential Tremor | Tremor control | 80–90% |
Dystonia | Symptom improvement | 50–70% |
What are Factors Affecting DBS Surgery Success Rate?
- Patient selection: Better results in medication-responsive symptoms (especially tremor). Lower outcomes in severe gait, speech, or balance problems.
- Age & cognitive health: Younger, cognitively healthy patients do better; advanced dementia lowers success.
- Electrode accuracy: Precise placement in target areas is critical for optimal results.
- Surgical expertise: High-volume, specialized centers achieve better outcomes and fewer complications.
- Post-surgery programming: Regular adjustments of stimulation settings strongly impact long-term success.
- Device & biological factors: Hardware issues (battery, wire problems) or infection can reduce effectiveness.
- Patient expectations: Realistic expectations improve satisfaction, since DBS improves symptoms but does not cure the disease.
Why Choose Turkey for Deep Brain Stimulation in 2026?
1. Affordable DBS Surgery and All-inclusive Packages
By 2026, DBS procedures in the United States or the United Kingdom can range from $60,000 to $100,000; the cost in Turkey is typically between $21,000 and $28,000 bundled in all-inclusive packages that generally cover the device (electrodes and IPG), surgeon and hospital fees, imaging MRI and CT scans, hospital stay, and airport or VIP transfers.
2. Board Certified Neurosurgeons with Multidisciplinary Team
Turkey is home to elite specialists in Deep Brain Stimulation (DBS) who hold accreditations from the Turkish Board of Neurosurgery (TBN) and the European Board of Neurological Surgery (EANS).
Furthermore, our medical staff is affiliated with international elite organizations, including the World Society for Stereotactic and Functional Neurosurgery (WSSFN) and the International Parkinson and Movement Disorder Society (MDS). These affiliations ensure that every procedure aligns with the latest 2026 clinical protocols and technological advancements.
3. Advanced Medical Technology
In Istanbul, neurosurgery hospitals use modern neurosurgical technology, and modern DBS systems include directional leads, rechargeable implantable pulse generators (IPGs), and intraoperative techniques such as microelectrode recording (MER).
4. Minimal Waiting Time, Fast Access & Centered Geographical Location
Unlike many public healthcare systems, where DBS surgery may involve long waiting lists, patients in Turkey can access treatment much faster. Additionally, Turkey’s geographic location between Europe, Asia, and the Middle East makes it easily accessible for international patients, further supporting its role as a global medical hub.
5. International Accreditation and Patient Safety
Many top hospitals in Turkey are accredited by international accreditations like JCI, ISO 9001, ensuring adherence to strict global healthcare standards, ensuring high levels of patient safety, surgical protocols, hygiene, and clinical quality comparable to leading hospitals in the United States and Europe.
Trust Turkey Luxury Clinics for Precise DBS Surgery and Close Monitoring
Contact Turkey Luxury Clinics today to receive a personalized DBS evaluation and connect with board-certified neurosurgeons specializing in movement disorders. Book a free consultation now.







.webp)
.webp)
.webp)
.webp)

