- What is IVF?
- What is Preimplantation Genetic Testing (PGT)?
- Can You Choose Gender with IVF? Medical and Law Perspectives
- Medical Reasons for Gender Selection
- How IVF Gender Selection Works (Step-by-Step)
- How IVF Gender Selection Works (Step-by-Step)
- IVF Success Rates & Clinical Evidence
- How Early Can You Know Baby’s Gender?
- Cost of IVF with Gender Selection in Different Countries 2026 Prices
- Non-PGT Gender Selection Alternative
- What Can You Choose with IVF?
- Why Turkey for Gender Selection IVF?
- FAQs About Can You Choose Gender with IVF
Can you choose your baby’s gender with IVF? Medically, yes, through advanced genetic testing, gender selection is possible with extremely high accuracy. However, its use is strictly regulated worldwide and is typically limited to specific medical indications rather than personal preference.
In vitro fertilization (IVF), combined with preimplantation genetic testing (PGT), has transformed reproductive medicine by allowing specialists to analyze embryos before implantation. This makes it possible not only to detect genetic disorders but also to identify the embryo’s sex at an early stage.
Accurate medical insights into how IVF gender selection works, its clinical accuracy, and how legal frameworks differ globally, especially in countries like Turkey, where the procedure is strictly regulated and permitted only for medical indications.
What is IVF?
In Vitro Fertilization (IVF) is a complex, multi-stage medical procedure in which eggs are fertilized by sperm outside the body in a controlled laboratory environment. The resulting embryo is then transferred into the uterus to achieve pregnancy.
The process involves a series of carefully timed steps, allowing specialists to monitor fertilization and early embryo development before implantation.
How the IVF Process Works (Step-by-Step)
The IVF procedure and timeline follow a structured and time-sensitive clinical sequence:
- Ovarian stimulation (10–14 days) to produce multiple eggs
- Egg retrieval (single-day procedure) performed under light sedation
- Fertilization (same day) using IVF or ICSI in a laboratory setting
- Embryo development (3–5 days) under controlled lab conditions
- Embryo transfer (Day 3–5) into the uterus at the optimal stage
Each stage is closely monitored to maximize implantation success.
Medical Conditions Treated with IVF
Clinically, IVF is used to treat infertility, particularly in cases where natural conception is not possible, such as blocked or absent fallopian tubes, severe male factor infertility, endometriosis, or age-related decline in fertility.
By bypassing key biological barriers, IVF allows direct control over fertilization and early embryo development, increasing the chances of successful implantation.
IVF is recommended in cases such as:
- Blocked or damaged fallopian tubes
- Severe male infertility (low sperm count or motility)
- Endometriosis
- Ovulation disorders
- Age-related decline in fertility
- Unexplained infertility
IVF Success Rates
IVF success rate depends mainly on maternal age and embryo quality:
- Under 35: ~50–55% live birth rate per cycle
- Age 35–37: ~40–45%
- Age 38–40: ~30–35%
- Over 40: ~10–20%
Success rates vary based on maternal age, embryo quality, and overall reproductive health, with higher success typically seen in younger patients. Success rates may improve when genetically tested embryos are used.
IVF Cost 2026
The cost of IVF typically ranges from $8,000 to $25,000 per cycle globally, depending on the clinic, country, and complexity of the treatment, with additional costs for advanced procedures such as ICSI or genetic testing.
What is Preimplantation Genetic Testing (PGT)?
According to leading reproductive medicine guidelines, including the American Society for Reproductive Medicine (ASRM), PGT is considered a highly reliable method for embryo selection when performed in accredited fertility laboratories.
Preimplantation Genetic Testing (PGT) is an advanced laboratory technique used during IVF to examine embryos for chromosomal or genetic abnormalities before they are transferred into the uterus. Its main goal is to select embryos that are genetically normal (euploid), improving the chances of a healthy pregnancy and reducing the risk of miscarriage or inherited genetic disorders.
There are three main types of preimplantation genetic testing:
- PGT-A: Screens for chromosomal abnormalities (most common use)
- PGT-M: Detects specific single-gene disorders
- PGT-SR: Identifies structural chromosomal rearrangements
PGT test allows specialists to identify:
- Chromosomal abnormalities (aneuploidy)
- Genetic disorders
- Sex chromosomes (XX or XY), when relevant
By selecting chromosomally healthy embryos, PGT can significantly improve implantation rates and reduce pregnancy loss.

Can You Choose Gender with IVF? Medical and Law Perspectives
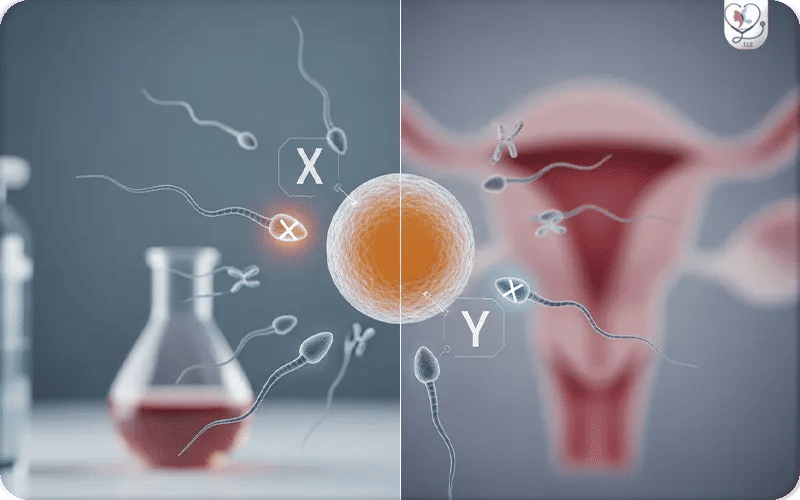
Yes, gender selection is scientifically achievable with nearly 100% accuracy. From a clinical standpoint, the process is performed using Preimplantation Genetic Testing (PGT-A) by which a cell is biopsied (taken precisely) from each embryo to check its chromosomes (XX for female, XY for male) before implantation, allowing doctors to transfer only embryos of the desired sex. .
After the fertilization of eggs in the lab, embryos are grown to the blastocyst stage (Day 5). Specialist embryologists then perform a trophectoderm biopsy to analyze the chromosomal makeup (XX for female, XY for male). This procedure not only identifies the biological sex but also ensures the embryo is chromosomally healthy (Euploid), significantly increasing the chances of a successful pregnancy and reducing miscarriage risks.
The Legal View About Gender Selection Permission in IVF (2026 Updates)
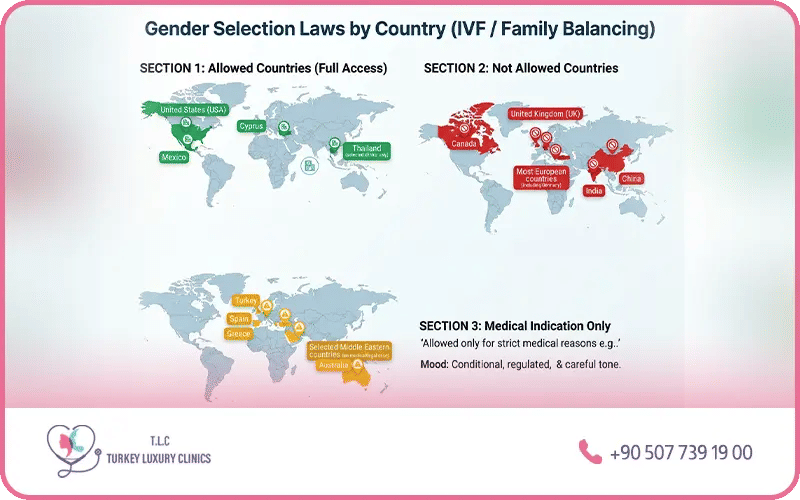
Legally, gender selection is categorized into two types: Family Balancing (non-medical) and Medical Necessity (to prevent genetic diseases).
Gender selection in IVF is legal in the United States, allowing for both medical necessity (preventing genetic diseases) and non-medical "family balancing".
Conversely, many countries, including Canada, China, and most of Europe, prohibit elective sex selection.
While sex selection via IVF is legally permitted in the United States, the American Society for Reproductive Medicine (ASRM) states that its non-medical use remains ethically controversial and should not be actively encouraged
In Turkey, gender selection is legally permitted for medical reasons only, specifically to prevent the transmission of serious sex-linked hereditary disorders (e.g., Hemophilia or Duchenne Muscular Dystrophy).
Medical Reasons for Gender Selection
- Duchenne muscular dystrophy
- Hemophilia
- X-linked disorders
Couples use gender selection during IVF primarily for two reasons: to prevent sex-linked genetic disorders and for family balancing, wanting an equal mix of boys and girls, or to have a specific gender first/last. Other motivations include emotional preparedness, cultural preferences, or to cope with the loss of a child by having another of the same sex.
Preventing Sex-Linked Diseases. Many serious genetic conditions are carried on the X chromosome and predominantly affect males, such as hemophilia, Duchenne muscular dystrophy, or color blindness. By selecting female embryos (XX), parents can eliminate the risk of passing these disorders to a son.
Beyond sex-linked diseases, PGT can also screen embryos for specific genetic mutations or single-gene disorders, helping parents select embryos free of known hereditary conditions, though this depends on the availability of genetic testing for the specific genes

How IVF Gender Selection Works (Step-by-Step)
Gender is determined during a blastocyst biopsy on Day 5 or 6 after fertilization, when the embryo has about 100 cells, allowing safe and accurate genetic testing.
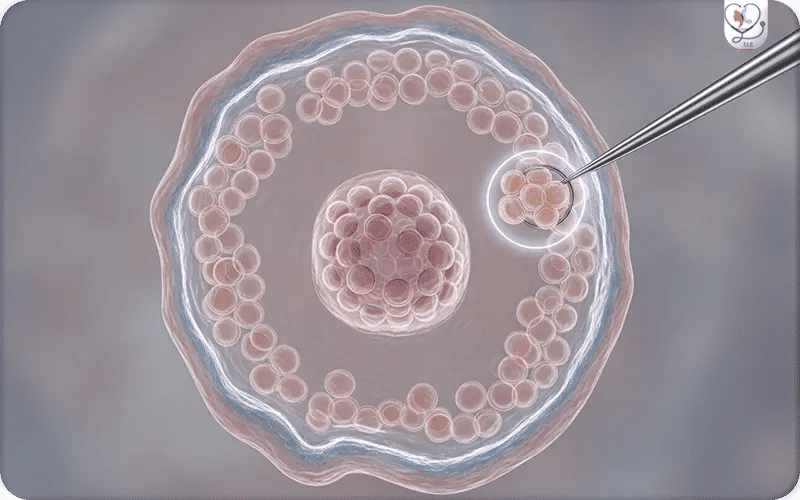
At this stage, the embryo has developed enough cells to provide a reliable sample without harming its potential to implant and grow. The cells are taken from the trophectoderm, the outer layer that later forms the placenta, while the inner cell mass—which develops into the baby—remains untouched.
Performing the biopsy too early may not yield enough cells for accurate testing, while waiting too long could delay the embryo transfer process. This timing ensures both safety and high accuracy in determining the embryo’s sex.
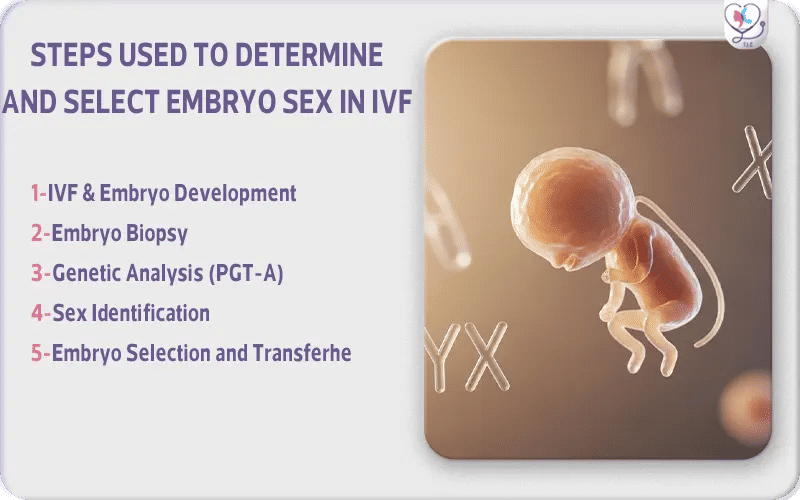
How IVF Gender Selection Works (Step-by-Step)
1. IVF and Embryo Development: Eggs fertilized with sperm in a laboratory reach the blastocyst stage (Day 5–6) or contain (100–150) cells.
2. Embryo Biopsy: Around 5 to 10 cells are taken from the trophectoderm, the outer layer that later forms the placenta, while the inner cell mass—which develops into the baby—remains untouched.
3. Genetic Analysis (PGT-A): The biopsied cells are analyzed using advanced technologies such as Next-Generation Sequencing (NGS).
4. Sex Identification: Based on the genetic results, XX chromosomes are Female and XY chromosomes are Male
5. Embryo Selection and Transfer: A chromosomally normal (euploid) embryo of the desired sex may then be selected for transfer into the uterus.
IVF Success Rates & Clinical Evidence
Preimplantation Genetic Testing (PGT-A) used during IVF offers nearly 100% diagnostic accuracy in identifying embryo sex chromosomes (XX or XY) before implantation under controlled laboratory conditions.
This is because the test directly analyzes the embryo’s chromosomes, identifying whether it carries XX (female) or XY (male) genetic material before it is transferred to the uterus.
IVF success is highly dependent on embryo chromosomal health (euploidy), which declines with maternal age. Clinical data from assisted reproductive technology registries demonstrate a clear reduction in euploid embryos as age increases:
Maternal Age | Euploid Embryos (Chromosomally Normal) | Impact on Gender Selection |
Under 35 | ~60% - 70% | High probability of multiple embryos of both genders. |
37 - 40 | ~35% - 45% | Moderate chance; may require more than one IVF cycle. |
Over 42 | <15% | Lower chance; fewer embryos available for screening. |
Source: Society for Assisted Reproductive Technology (SART) National IVF Data Reports
Peer-reviewed clinical studies and meta-analyses published in journals such as Reproductive Biology and Endocrinology and Fertility and Sterility demonstrate that the transfer of euploid embryos significantly improves implantation and live birth rates while reducing miscarriage risk compared to untested embryos.
Additionally, the outcome of gender selection depends on the availability of euploid embryos of the desired sex, which is influenced by maternal age, egg quality, and sperm health:
- The number of euploid embryos depends mainly on maternal age.
- As maternal age increases, the risk of chromosomal abnormalities in eggs increases.
- This leads to a lower number of chromosomally normal (euploid) embryos available for testing.
- Egg quality directly affects the chances of producing healthy embryos suitable for selection.
- Sperm quality can also influence early embryo development.
- Fewer euploid embryos reduces the likelihood of having embryos of the desired sex available for selection.
How Early Can You Know Baby’s Gender?
The earliest option is non-invasive prenatal testing (NIPT), which can detect the presence of a Y chromosome through a simple blood test as early as 10 weeks of pregnancy. This method is highly accurate but is primarily used to screen for genetic conditions, not only for sex determination.
Another common method is the second-trimester ultrasound scan, usually performed between 18 and 21 weeks. During this anatomy scan, the technician may be able to identify the baby’s sex based on visible genital development, depending on the baby’s position. However, this method is not always 100% accurate, and in some cases, the sex cannot be clearly determined.
In more specific medical situations, procedures such as amniocentesis or chorionic villus sampling (CVS) can also reveal the baby’s sex, typically between 11 and 16 weeks. Still, these tests are usually recommended only when there is a medical reason, given their invasive nature.
For couples undergoing IVF with Preimplantation Genetic Testing (PGT-A), the baby’s sex can be identified at the embryo stage (Day 5–6) before pregnancy even begins, making it the earliest and most precise method available.
Despite these options, it is important to note that the only completely guaranteed way to know a baby’s sex with absolute certainty is at birth.
Cost of IVF with Gender Selection in Different Countries 2026 Prices
Country | IVF (Egg Retrieval + Transfer) | PGT (Genetic Testing) | IVF + PGT Total Cost |
United States | $15,000 – $25,000 | $5,000 – $10,000 | $20,000 – $35,000+ |
Turkey | $3,000 – $5,000 | $1,500 – $3,500 | $5,000 – $8,500 |
Cyprus | $5,000 – $8,000 | $2,000 – $4,000 | $8,000 – $12,000 |
Spain / Greece | $4,000 – $7,000 | $2,000 – $3,500 | $6,000 – $10,000 |
IVF with preimplantation genetic testing (PGT) costs vary significantly depending on the country, clinic standards, and laboratory technology used.
The United States remains the most expensive option due to advanced medical infrastructure and higher laboratory fees, while European destinations such as Spain and Greece offer moderate pricing under strict regulatory frameworks.
In contrast, Turkey and Cyprus have become leading fertility destinations due to their lower overall costs combined with access to modern IVF laboratories and experienced embryology teams.
In most cases, the total price includes ovarian stimulation, egg retrieval, fertilization, embryo culture, and transfer, while PGT is calculated separately as an additional genetic analysis cost that depends on the number of embryos tested and the type of screening required.
Non-PGT Gender Selection Alternative
Method | Accuracy | Cost | Timeline | Legal Status |
IVF + PGT | 99% | High | 2–4 weeks | Restricted/Medical |
Natural Conception | 50% | Low | Natural | Legal |
Adoption | N/A | High | Months/Years | Legal |
1. MicroSort
This method uses a process called flow cytometry to sort sperm based on DNA content (X-sperm contains approximately 2.8% more DNA than Y-sperm).
Sperms are stained with a fluorescent dye. X-sperm emits a brighter signal and is separated from Y-sperm. This method is not FDA-approved for clinical use in the United States. and outside the legal clinical framework in many strictly regulated countries like Turkey and the UK due to its experimental nature
2. Ericsson Method
One of the oldest and most affordable techniques, based on differences in sperm motility.
Sperm are placed over layers of albumin (a protein). Faster-swimming Y-sperms are collected from the lower layers.
Many experts question its reliability, as outcomes may not significantly exceed the natural 50/50 probability.
What Can You Choose with IVF?

With IVF, you can choose your baby's biological sex (gender), select embryos free from specific genetic diseases and more options that can be added to standard IVF according to parents desire using Preimplantation Genetic Testing (PGT)
There are two main types of PGT: PGT-A, which checks chromosome numbers and also identifies sex, and PGT-M/SR, which looks for single-gene or structural chromosome disorders and can reveal sex if needed.
1. Sex/Gender Selection:
Using Preimplantation Genetic Testing (PGT), doctors can analyze embryos for sex chromosomes (XX for female, XY for male) and select one for transfer. This is often done to prevent sex-linked diseases or for family balancing, though it remains ethically debated.
2. Genetic Health:
PGT can screen embryos for serious genetic conditions (e.g., cystic fibrosis, Huntington’s disease) and chromosomal abnormalities, allowing the selection of the healthiest embryos.
3. Gestational Carrier:
Couples can choose a gestational carrier (surrogate) to carry the pregnancy.
4. Number of Embryos:
You can decide to transfer one or multiple embryos, affecting the chance of twins or triplets.
5. Fertilization Method:
You may select standard IVF or Intracytoplasmic Sperm Injection (ICSI) depending on fertility needs.
Why Turkey for Gender Selection IVF?
Turkey operates under a strictly regulated legal framework for IVF and preimplantation genetic testing (PGT), where all procedures are performed within licensed medical institutions under official health authority supervision. The system is designed to ensure that genetic testing and embryo-related procedures are conducted in a controlled clinical environment, not in unregulated settings.
Gender selection is permitted only for medical indications, such as preventing serious genetic and sex-linked disorders, and is not allowed for personal or non-medical preference. This regulatory structure helps maintain clear ethical boundaries in reproductive medicine.
The Turkish fertility system also plays an important role in preventing unregulated or black-market practices, as all IVF and genetic testing procedures must be performed in approved clinics that follow national medical standards and laboratory regulations.
Compared to non-regulated environments, Turkey’s approach ensures that IVF treatments are delivered under legal oversight, standardized protocols, and clinical accountability, supporting patient safety and medical integrity.
For patients seeking personalized evaluation , Turkey Luxury Clinics provides coordination with experienced fertility specialists to help determine eligibility, explain available genetic testing options, and support treatment planning under clinical supervision.







.webp)
.webp)
.webp)
.webp)

